(The following is the second in a series of responses between Dr. Arencibia-Albite and myself. The impetus for this little point-counterpoint is a column I had published in Alan Aragon’s Research Review [AARR] back in January. In that article, I strongly analyzed the underlying assumptions of a manuscript put forth by Dr. Arencibia-Albite on a pre-print server [which I describe below]. I highly encourage everyone to read the manuscript, as well as my piece and Dr. Arencibia-Albite’s response before continuing [links are provided for each below]. For those who are not subscribers to AARR, I do give a brief recap of my position below and Dr. Arencibia-Albite also points out various sections of my article in his reply. Worth noting is the facetious tone of the piece I contributed to AARR—which leads me to begin with the following…)
An olive branch
First, I would like to thank Dr. Arencibia-Albite for responding to some of the points I raised in my recent commentary in the January issue of Alan Aragon’s Research Review (AARR). I realize the tone of my piece was on the facetious side and I do apologize if it came off as “hostile” and “ridiculing”. That was not my intention—the piece was simply meant to be a fun, non-academic, non-sterile editorial for readers. I hope a collegial hand can be extended in mutual friendship and dialogue (be it heated at times).
Now, on to the good stuff!
Recap of my position
I want to quickly recap my position for those who might be stumbling upon our back-and-forth just now. Your model (the Mass Balance Model [MBM]) is certainly thought-provoking and provocative—which is what drew me to the manuscript in the first place. It purports to challenge the firmly established Energy Balance Equation that states that body energy stores are the mathematical difference between energy intake and energy expenditure. As you stated, while the MBM does not intend to promote one style of eating over another, it does predict that diets with lower mass will result in greater changes in body weight/fat than diets with higher mass, despite being similar in calories. You then reference a host of trials in support of this contention. These studies apparently show that a low-carbohydrate diet outperforms an isocaloric, low-fat diet (with higher mass) for weight/fat loss [1-6]. It is these very studies that I critiqued in my AARR piece, showing the limitations of the studies—i.e. how they were either poorly controlled, relied solely on self-reported diet records, lacked accurate body composition measures, or all of the above. Consequently, this lead me to question the veracity of the observation that a low-carbohydrate diet is superior for weight/fat loss. (I will get to the Hall et al. paper in a second since much hinges on that paper in my opinion.)
Therefore, while you state that your model does not intend to support one diet over another (point taken), it is predicated on the underlying observation of the superiority of low-carbohydrate diets, which, in my opinion, is miles away from a firm observation. This is one place where we significantly differ.
Kong et al. 2020
Before addressing the Hall study, I want to first comment on another trial that you bring up in your response to me and that you modeled in your manuscript, stating that the MBM predictions match “perfectly” the data from this study (i.e. Kong et al. 2020 [7]).
It is from this reference that I have come to realize perhaps the biggest difference between you and I when analyzing the relevant literature—you (in my opinion) appear to have a very high degree of confidence in self-reported dietary intake records whereas I simply do not. Here is why.
It has been firmly established that individuals habitually and significantly underreport their true energy/nutrient intakes in free-living trials that rely on self-reported food records for dietary control. To quote a recent systematic review that examined the accuracy of dietary reporting (e.g. food records) when compared to the doubly labeled water (DLW) method [8]:
“Of the studies that reported the accuracy of food records at the group level, the majority of studies (n=19) found significant underreporting of EI [energy intake], by 11 to 41% […] with over-reporting found in only one study by 8% […] Three studies found no significant difference between absolute EI estimated by food record and TEE [total energy expenditure] measured by DLW.”
In other words, self-reported dietary intake data is probably the most unreliable data you could ever wish to find. Nonetheless, you continually rely upon this category of dietary trial—of which Kong et al. falls into—to make your points and model your predictions. I respectfully disagree with the assumption that the data presented in these types of trials is worthy of modeling. Therefore, while they may support your model, I find them horribly flawed (as was my initial position in AARR). Here is where we significantly differ again.
Hall et al. 2015
With regard to this very important study, you correctly point out in your response to me that the changes in fat mass between the two diets is statistically identical (although I never said that they were statistically significantly different), with both groups showing similar fat mass losses (-0.529 kg in the carbohydrate restricted group vs. -0.588 kg in the fat restricted group). As you can see—and to clarify—my point is that if the carbohydrate restricted diet were superior to the fat restricted diet, it would have led to a greater fat mass loss, as per the MBM predictions. This, as you pointed out, was not the case.
You then pivot by calculating fat balance based on the DEXA-derived losses in body fat (and I have no arguments with your math as presented) showing a greater net negative fat balance with the carbohydrate restricted arm. However, it is here where I think you need to square two incompatible pieces of information:
If you believe the DEXA measures to be THAT accurate, then despite your calculations, the fat restricted arm still lost more body fat during the trial.
If you recognize the limitations of DEXA—given the short study duration and small changes in fat mass (i.e. near limitations of the machine, as Hall et al. point out in their discussion)—and therefore calculate fat balance based on calorimetry measures (as Hall did), then the fat restricted diet had a greater net negative fat balance than the carbohydrate restricted diet (-89 g/d vs. -53 g/d, respectively).
Therefore, either you really trust the DEXA measures, in which case fat restricted won out, regardless of the math, or, you recognize its limitations and calculate fat balance based on calorimetry (as Hall did)—where again, fat restricted still won out. I realize the study was very short, and that is a perfectly debatable point (I personally feel it is a huge limitation)—but it, nevertheless, does not support predictions made by the MBM.
A closer look at Horton et al. 1995
Leaving everything already mentioned aside, let us assume that the MBM is valid. The prediction based on this model should also hold true in other conditions such as overfeeding. As pointed out by Alan toward the end of my AARR piece, the MBM fails to live up to predictions in all caloric states—let us currently stick with overfeeding since you mentioned the following study explicitly in your response.
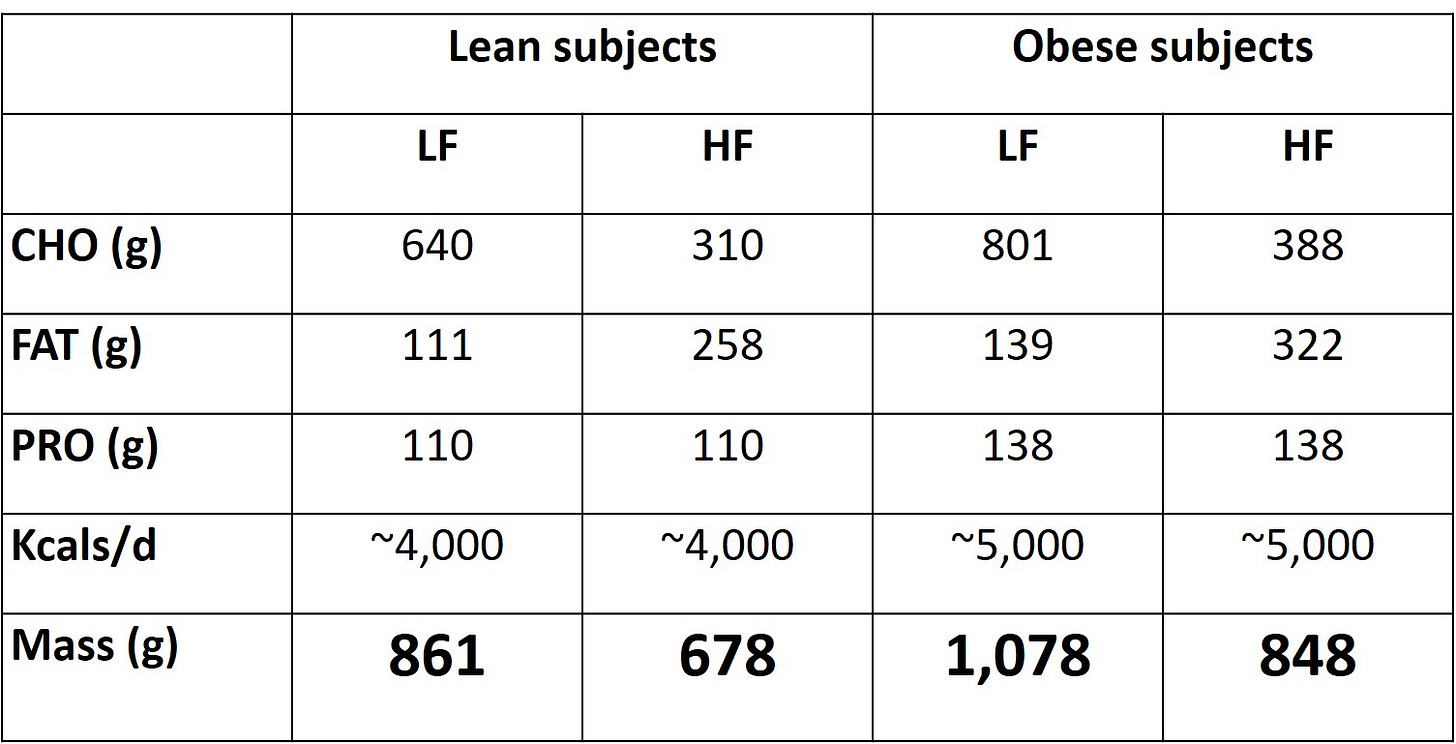
To demonstrate: As per the MBM, it is predicted that a higher-carbohydrate diet that contains, say, ~4,000 calories (64% CHO, 25% FAT, 11% PRO) should result in greater changes in body weight than a lower-carbohydrate diet with ~4,000 calories but a lower mass (31% CHO, 58% FAT, 11% PRO). I do not believe this to be an accurate prediction given that is has already been tested and shown to be false.
Indeed, Horton et al. overfed lean and obese subjects 150% of their caloric requirements, with the additional 50% of calories coming from fat or carbohydrate [9]. (It also controlled for protein intakes making this study very valuable in my opinion.) Given the equal calories but different masses of the diets (see table below), we should predict less weight/fat gain on the lower carbohydrate, higher fat (and therefore lower mass) diet, as per the MBM.
Breakdown of the overfeeding diets
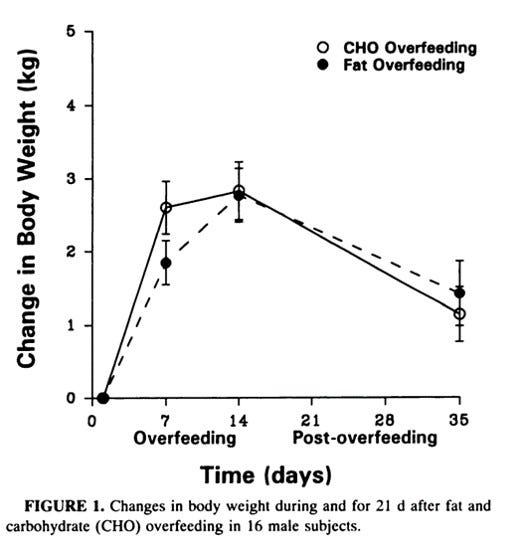
Despite the predictions of the MBM, after 14 days of overfeeding, both groups gained equivalent body mass (figure below).
You countered by stating the limitation of the study duration (fair enough), implying that a statistical difference would perhaps emerge after 2 weeks. My question is: “in what sense?” It is clear that the higher-fat condition quickly approached the higher-carbohydrate condition by 2 weeks and that the trajectories imply the higher-fat condition surpassing the higher-carbohydrate conditions.
Further, if we look at changes in body fat (table below), the higher-fat, lower-carbohydrate (and lower mass) protocol actually led to slightly more body fat than the higher-carbohydrate (thus, higher mass) protocol (+1.51 kg vs. +1.48 kg, respectively)—albeit trivially so and within the detection limits of underwater weighing. Regardless, and more to the point, the diet higher in fat and lower in carbohydrate most certainly did not lead to less weight or body fat gain despite containing similar calories but less mass.
(I will note, however, if you parse out the subjects based on lean/obese status, you can see leaner subjects did slightly better on higher-carb whereas the obese subjects did slightly better on higher-fat—but again, the differences are extremely trivial and within the detection limits of the body composition method.)
Thus, the present overfeeding study also fails to confirm the predictions of the MBM. Indeed, numerous trials in all energy states show similar results (as already indicated in the AARR piece [10-12]).
Correcting arithmetic
I would be remiss if I did not also respond to a point you made regarding the following (that Alan himself actually contributed to the piece):
“If it was all about mass balance and not energy balance […] then controlled overfeeding studies would show LESS weight/fat gain with the fat-dominant energy surpluses. More explicitly, 44% less grams of fat are required to equal the caloric load of carbohydrate grams (carbohydrate = 4 kcal/g, fat = 9 kcal/g), so less nutrient mass is present in the higher-fat condition.”
In your response, you correctly corrected the math and showed that it actually requires 56% less fat to equal the caloric load of carbohydrate—thus, making his point stronger given the findings in overfeeding studies—i.e. similar gains in body weight/fat. (Alan assured me that it was a “hasty mistake” on his part and that he will be changing the math in the AARR article. He thanks you for pointing it out and I also apologize for not crunching the numbers myself when proofing the piece.)
In closing
Everything considered I am nevertheless always open to more, direct testing of the MBM with longer, well-controlled trials. I would never argue that testing of a potentially viable model to understand body weight management should not occur. Science is an open-ended game, and I philosophically share your willingness to challenge dogma. As it stands, however, given my read of the literature, and the statements put forth in my original piece and now here, I still feel the MBM fails to better explain changes in body weight/fat than good old, boring energy balance.
Best!
References
1. Lean, M.E., et al., Weight loss with high and low carbohydrate 1200 kcal diets in free living women. Eur J Clin Nutr, 1997. 51(4): p. 243-8.
2. Samaha, F.F., et al., A low-carbohydrate as compared with a low-fat diet in severe obesity. N Engl J Med, 2003. 348(21): p. 2074-81.
3. Brehm, B.J., et al., A randomized trial comparing a very low carbohydrate diet and a calorie-restricted low fat diet on body weight and cardiovascular risk factors in healthy women. J Clin Endocrinol Metab, 2003. 88(4): p. 1617-23.
4. Brehm, B.J., et al., The role of energy expenditure in the differential weight loss in obese women on low-fat and low-carbohydrate diets. J Clin Endocrinol Metab, 2005. 90(3): p. 1475-82.
5. Bazzano, L.A., et al., Effects of low-carbohydrate and low-fat diets: a randomized trial. Ann Intern Med, 2014. 161(5): p. 309-18.
6. Hall, K.D., et al., Calorie for Calorie, Dietary Fat Restriction Results in More Body Fat Loss than Carbohydrate Restriction in People with Obesity. Cell Metab, 2015. 22(3): p. 427-36.
7. Kong, Z., et al., Short-Term Ketogenic Diet Improves Abdominal Obesity in Overweight/Obese Chinese Young Females. Front Physiol, 2020. 11: p. 856.
8. Burrows, T.L., et al., Validity of Dietary Assessment Methods When Compared to the Method of Doubly Labeled Water: A Systematic Review in Adults. Front Endocrinol (Lausanne), 2019. 10: p. 850.
9. Horton, T.J., et al., Fat and carbohydrate overfeeding in humans: different effects on energy storage. Am J Clin Nutr, 1995. 62(1): p. 19-29.
10. Lammert, O., et al., Effects of isoenergetic overfeeding of either carbohydrate or fat in young men. Br J Nutr, 2000. 84(2): p. 233-45.
11. Hall, K.D. and J. Guo, Obesity Energetics: Body Weight Regulation and the Effects of Diet Composition. Gastroenterology, 2017. 152(7): p. 1718-1727 e3.
12. Leibel, R.L., et al., Energy intake required to maintain body weight is not affected by wide variation in diet composition. Am J Clin Nutr, 1992. 55(2): p. 350-5.