“La vie est donc une combustion” - Antoine Lavosier
Introduction
In Part 1 of this series, we covered a whole host of topics related to energy balance and energy intake; to recap everything here would take too long. So, if you are just joining, I encourage you to brush up on the previous column before continuing on, here.
With that said, I do want to start with reiterating that the Energy Balance equation states:
Changes in energy stores = Energy intake – Energy expended
Thus, any mismatch between energy expended and energy ingested (digested and absorbed) will result in changes in body energy stores (i.e. glycogen and fat). Having covered energy intake, we now cover energy expenditure.
Energy expenditure
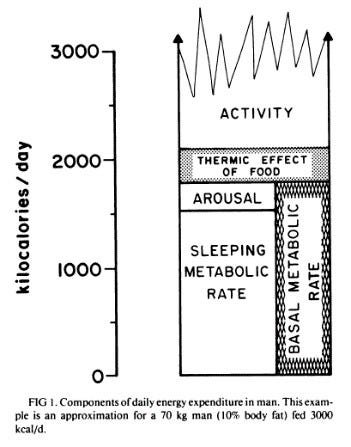
Your body spends energy on a variety of processes primarily related to cellular metabolism and physical activity. If we expand upon this foundation, we have four measurable components that comprise total daily energy expenditure (TDEE; see figure below). These are: basal metabolic rate (BMR), the thermic effect of food (TEF), the energy expended during activity, which encompasses both the energy cost of exercise (EEx) and non-exercise activity thermogenesis (NEAT) [1].
Notice how some of these terms have the word ‘thermic’ or ‘thermogenesis’ in their name. This alludes to the fact that metabolism is (horribly) inefficient and much of the potential energy in nutrients that could have been transferred to the bonds of ATP is wasted as heat. (Which can be measured! More on this later.)
Basal Metabolic Rate (BMR)
Starting with the largest portion of a persons’ TDEE, BMR is, as its name implies, the sheer minimum energy requirements for basic cellular metabolism. (Keeping the lights on, so to speak [i.e. keeping the sodium-potassium pump going and maintaining ion concentration gradients throughout the body, etc.]) On average, this amounts to ~60% of TDEE (at least in those who are not super active).
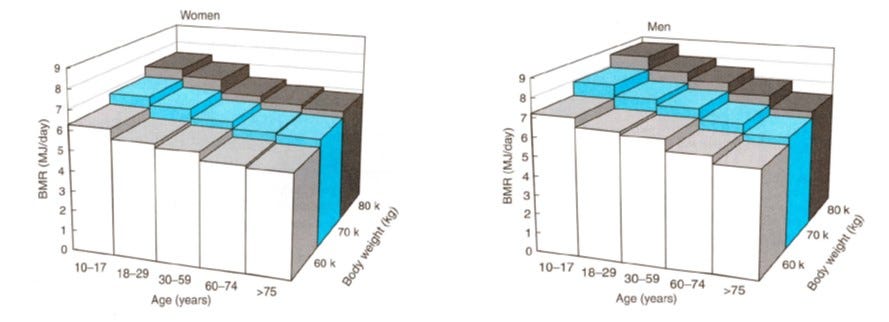
Harkening back to my piece on body composition, you will remember that lean body mass is the primary driver (i.e. it accounts for ~75%) of your BMR—and no, not your skeletal muscle (which is fairly metabolically inactive at rest [2]), but your organs such as brain, liver, heart and kidneys [2]. To put this into perspective, skeletal muscle contributes approximately 13 kcal/kg per day of metabolic activity, whereas your liver, brain, heart and kidneys contribute between 200-400 kcal/kg [2]…each! Thus, larger individuals, of both sexes, will have higher BMRs due to proportionally greater lean body mass. This, however, tends to decrease with age. (See figures below.)
Thermic effect of food (TEF)
While we already covered TEF in Part 1—at least cursorily when we discussed energy intake and noted that TEF (also known as diet-induced thermogenesis [DIT]) is the increased energy cost of digesting, absorbing and metabolizing the nutrients from the diet. While commonly averaged out to approximately 10% of total caloric intake, TEF is mostly dependent upon the nutrient composition of the diet and meal size [3, 4] although other factors such as aerobic fitness have been shown to impact TEF [5].
With regard to macronutrient composition, protein, carbohydrate and fat have varying thermogenic potential, with protein having the highest cost (~20-30%), followed by carbohydrate (5-6%) and fat (0-3%) [6]. Of interest: this is merely one reason higher protein intakes are suggested during weight loss diets—in addition to the satiating effects of protein that increase the chances for dietary adherence coupled with its ability to preserve lean tissue [7].
Energy expended during exercise (EEx)
Simply, this is the energy expended during structured physical activity (i.e. exercise). Obviously, this can be quite variable: If you don’t engage in exercise very often or just live a sedentary, non-active lifestyle, your EEx will be quite low (~10-15% of TDEE). On the other hand, if you are very active, such as a runner, swimmer, or cyclist, EEx can be as high as 30-50% of TDEE. Further, body size also affects the cost of locomotion with (you guessed it) larger bodies being more energetically costly than smaller bodies [8]. (This, in part, is one reason why women, who tend to have smaller bodies, need to engage in what seems like endless amounts of cardio just to lose a trivial amount of weight.)
Non-exercise activity thermogenesis (NEAT)
This is where the magic happens! NEAT is the energy cost of everything else that isn’t structured physical activity: leisure, sitting, postural changes, walking, fidgeting, handwashing dishes, getting up to change the channel (for those old enough to remember). Things like that. Given the seemingly endless number of things that fall under the category of NEAT, it is no surprise that it is the single most variable aspect of energy expenditure. And, unfortunately, it is likely biologically determined.
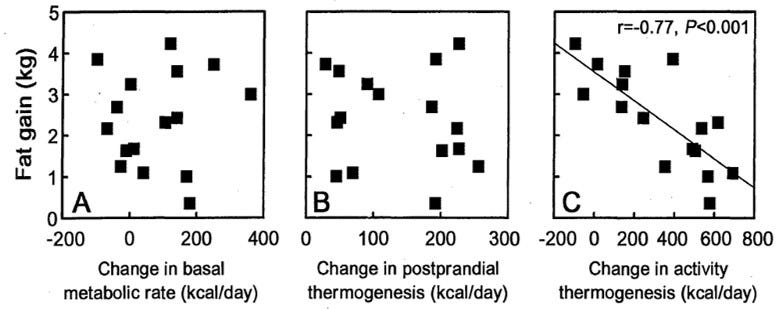
To illustrate the power of NEAT, we turn to the seminal study by James Levine and company [9]. In this trial, 16 subjects were recruited to a metabolic ward and overfed by 1,000 calories per day for eight weeks. By the end of the trial, some subjects gained plenty of weight whereas others gained next to none—certainly not as much as they could/should have! The range of weight gain was 1.4-7.2 kg over the 8-week period, with some subjects gaining greater than 4 kg of body fat and others less than 1 kg.
What accounted for such differences? Not changes in BMR, not changes in TEF. You guessed it, NEAT! The subjects who resisted weight and fat-gain moved a heck of a lot more than those who packed on the pounds (see figure below). Some subjects even responded by moving less than they initially did before the overfeeding period. (Very unfortunate.)
As I already mentioned, NEAT is likely biologically determined [10], meaning that you are predisposed to moving more or less in response to overeating. In turn, this decreases or increases your risk of weight/fat gain, respectively—not the other way around (i.e. being obese causes you to move less and being lean causes you to move more.) Put another way, you are resistant to weight gain because you naturally move more, you are susceptible to weight gain because you naturally move less. This is the power of NEAT!
Methods to measure energy expenditure
At this point, we have covered every aspect that goes into energy intake and expenditure and I hope that you realize and appreciate that Energy Balance it is a lot more complicated than initially thought. (And don’t worry, it gets even more complicated once we start to consider what happens during overfeeding and underfeeding—yay!)
At this point, however, we still need to consider the ways in which energy expenditure can be measured. Like energy intake, the different methods have their strengths and limitations with some methods only capturing certain, or the summation of all, components of energy expenditure. Thus, for example, one method may not allow you to measure TEF but it can give you TDEE. Depending on the research question, this could be a huge limitation or an unimportant matter.
We will briefly consider the popular methods, what components of energy expenditure they actually measure, as well as their strengths and limitations now.
Prediction equations
While not a measure of energy expenditure, prediction equations (as their name implies) try to predict an individuals’ BMR. These equations take into account the individuals’ biological sex, age, weight and height and then use that information to calculate BMR. From there, a fudge factor is thrown in (as an estimate of physical activity) to get TDEE. While obviously limited, prediction equations are not completely inaccurate, and they at least provide an individual with a starting point from which to estimate caloric needs and plan diets accordingly. Popular equations are ones such as Harris-Benedict and Mifflin St. Jeor. Certain equations are more accurate for certain populations, but that is beyond what I want to talk about here.
Ultimately, if you have zero access to more accurate methods of assessing energy expenditure (described below), prediction equations are your best (and only) option.
Direct calorimetry
Remember when I briefly alluded to the fact that energy transfer is horribly inefficient and much of the potential energy that could have been transferred to the bonds of ATP is lost as heat? Direct calorimetry measures this heat production given that heat production is a function of energy transfer and ATP turnover—i.e. energy expenditure.
There are three principle types of direct calorimeters. Their differences are unimportant. Effectively, a direct calorimeter is a highly expensive room that subjects reside in for a prolonged period of time (up to 24 h) and the heat lost from their body is measured. The majority of heat lost from the body leaves in the form of radiative and convective losses. The remaining 20% or so comes from evaporative losses. (Conductive heat loss is trivial.)
While quite accurate, direct calorimetry is expensive, burdensome for the subject, and only gives TDEE—in the context of calorimetry confinement. (!) Indeed, when subjects’ TDEE is estimated using another method (doubly labelled water) that doesn’t require hours-worth of room confinement, energy expenditures are typically higher [11], indicating that the experimental conditions of direct calorimetry may not capture the true energy needs of people in their true habitats.
Indirect calorimetry
Indirect calorimetry implies the measurement of energy expenditure sans heat. This can be accomplished two ways: through gas exchange or via isotopically labeled water. First, gas exchange.
Just as heat production (i.e. loss) is tied to ATP production and therefore energy expenditure, oxygen (O2) consumption and carbon dioxide (CO2) production are similarly involved due to their requirement (O2) and production (CO2) during energy transfer. Thus, gas and heat exchange are coupled. Therefore, if we can measure the amount of gas being exchanged, we can calculate how much heat was lost and thus how much energy expended.
Indirect calorimeters come in all shapes and sizes. The two most common forms are the whole room indirect calorimeter and a facemask/ventilated hood. In the former, a subject resides in a room (anywhere from 5-24 h) and total gas exchange is measured over time. In the latter, a mask (or hood) is applied to the subjects face and gas exchange is measured in response to bedrest, exercise, or a meal. As such, the mask is applied for much shorter periods (~30 minutes).
In either situation, O2 and CO2 are measured and energy expenditure can be obtained from that exchange. The power of indirect calorimetry is that it can also be used to estimate the individual components of energy expenditure. In other words, you can parse out the relative contributions of BMR, TEF and activity. This is opposed to direct calorimetry, which can only measure TDEE.
Another strength of indirect calorimetry is that it can identify which fuels are being used by the body by creating a ratio of CO2 produced to O2 consumed. This is called the respiratory exchange ratio (RER for the exercise scientists) or the respiratory quotient (RQ for the nutrition scientists). A value of 1 indicates carbohydrate oxidation; a value of 0.7 indicates fat oxidation.
To illustrate the power of indirect calorimetry, let’s say you wanted to know how many calories you would expend during exercise, but also wanted to know which fuels you were using during that bout. Easy! You just come to the lab, I put the mask on your face and have you run on the treadmill while collecting your breath (gas) every few seconds. From this, we can estimate total calories burned as well as check the RERs measured every few seconds to see which fuels you were using throughout that bout of exercise. Very cool!
Doubly labeled water (DLW)
This method is based on the principle that the body elimination rates of hydrogen (H) and oxygen (O) are different, with oxygen being eliminated at a faster rate (see figure below). This is because oxygen is eliminated as both water (H2O) and carbon dioxide (CO2). Thus, if a known quantity of isotopically labelled (or heavy) water is given to an individual, allowed to equilibrate in the body, and then measured again following a known period, TDEE can be measured, as the difference in slopes is, by definition, the rate of CO2 lost [1, 12]. Thus, if CO2 elimination is known energy expenditure can be calculated. How cool!!
This method is highly reproducible, unbiased, and accurate under most normal conditions, with accuracy improving with more frequent fluid sampling post ingestion [1]. The drawback is that it only gives TDEE and not the individual components or fuel utilization.
Physiological observations
For completeness sake, I will mention briefly that there are other (less accurate) methods to estimate energy expenditure, particularly activity levels. These would fall into the realm of activity recalls, pedometers and accelerometers, and other various activity monitors. Nowadays many people have a Fitbit or an Apple Watch that monitors their every waking (and non-waking) moment. Perhaps they can be helpful for individuals in the sense of increasing the likelihood of moving more and improving health habits, but I am not going to put much stock in them, certainly not as accurate measures of energy expenditure. Indeed, depending on an individuals’ body size, accelerometers can drastically under- or overestimate true energy expenditure with little correlation when compared to DLW [13, 14].
Summing up
Next time we will (finally) cover how the Energy Balance equation changes in response to conditions such as overfeeding and underfeeding. The punchline being: the Energy Balance equation is not static, but is highly dynamic and changes according to the physiological energy state of the body. Until then, let us sum up today’s information:
There are four components of energy expenditure: BMR, TEF, EEx and NEAT
BMR is the basal metabolic activity of the body; it is driven largely by body size and lean body mass
TEF is energy cost of digesting, absorbing, and storing nutrients; it is largely driven by meal size and protein content
EEx is the energy cost of structure physical activity; it is largely driven by body size and activity levels (e.g. sedentary vs. athlete)
NEAT is the energy cost of all other, non-structured physical activity; this is likely biologically determined with some people being more predisposed to move more than others, thus increasing or decreasing the likelihood of gaining weight
Energy expenditure can be measured using a variety of methods; these are categorized as direct and indirect calorimetry, along with physiological observations such as activity monitors
Direct calorimetry measures energy expenditure via measuring heat production
Indirect calorimetry measures energy expenditure via measuring gas exchange or stable isotopes (i.e. doubly labeled water)
Gas exchange also can indicate fuel utilization by creating a ratio between expired CO2 and inspired O2 called RER or RQ; a value of 1 indicates CHO oxidation and 0.7 indicates FAT oxidation
References
1. Levine, J.A., Measurement of energy expenditure. Public Health Nutr, 2005. 8(7A): p. 1123-32.
2. McClave, S.A. and H.L. Snider, Dissecting the energy needs of the body. Curr Opin Clin Nutr Metab Care, 2001. 4(2): p. 143-7.
3. Quatela, A., et al., The Energy Content and Composition of Meals Consumed after an Overnight Fast and Their Effects on Diet Induced Thermogenesis: A Systematic Review, Meta-Analyses and Meta-Regressions. Nutrients, 2016. 8(11).
4. Calcagno, M., et al., The Thermic Effect of Food: A Review. J Am Coll Nutr, 2019. 38(6): p. 547-551.
5. Hill, J.O., et al., Meal size and thermic response to food in male subjects as a function of maximum aerobic capacity. Metabolism, 1984. 33(8): p. 743-9.
6. Acheson, K.J., Influence of autonomic nervous system on nutrient-induced thermogenesis in humans. Nutrition, 1993. 9(4): p. 373-80.
7. Cava, E., N.C. Yeat, and B. Mittendorfer, Preserving Healthy Muscle during Weight Loss. Adv Nutr, 2017. 8(3): p. 511-519.
8. Ferraro, R., et al., Energy cost of physical activity on a metabolic ward in relationship to obesity. Am J Clin Nutr, 1991. 53(6): p. 1368-71.
9. Levine, J.A., N.L. Eberhardt, and M.D. Jensen, Role of nonexercise activity thermogenesis in resistance to fat gain in humans. Science, 1999. 283(5399): p. 212-4.
10. Levine, J.A. and C.M. Kotz, NEAT--non-exercise activity thermogenesis--egocentric & geocentric environmental factors vs. biological regulation. Acta Physiol Scand, 2005. 184(4): p. 309-18.
11. Seale, J.L., et al., Comparison of doubly labeled water, intake-balance, and direct- and indirect-calorimetry methods for measuring energy expenditure in adult men. Am J Clin Nutr, 1990. 52(1): p. 66-71.
12. Schoeller, D.A., Insights into energy balance from doubly labeled water. Int J Obes (Lond), 2008. 32 Suppl 7: p. S72-5.
13. Plasqui, G. and K.R. Westerterp, Physical activity assessment with accelerometers: an evaluation against doubly labeled water. Obesity (Silver Spring), 2007. 15(10): p. 2371-9.
14. Leenders, N.Y., W.M. Sherman, and H.N. Nagaraja, Energy expenditure estimated by accelerometry and doubly labeled water: do they agree? Med Sci Sports Exerc, 2006. 38(12): p. 2165-72.